Osteoblast cytocompatibility and antibacterial effect of ginger main compounds
 ; Young-Seon Baek
; Young-Seon Baek ; Seo-Young Kim
; Seo-Young Kim ; Yu-Kyoung Kim
; Yu-Kyoung Kim ; Yong-Seok Jang
; Yong-Seok Jang ; Tae-Hwan Kim
; Tae-Hwan Kim ; Tae-Sung Bae
; Tae-Sung Bae ; Min-Ho Lee*
; Min-Ho Lee*
Abstract
Ginger has been used worldwide in traditional medicine. It has been reported that phenolic compounds such as gingerol and shogaol in ginger have beneficial cellular effect and antibacterial effect. The purpose of this study was to investigate the effect of gingerol and shogaol on the cytocompatibility for the osteoblastic cells and antibacterial activity against oral microorganisms. Chemical structures of gingerol and shogaol were determined by Fourier transform infrared (FT-IR). Thermal and pH stability was analyzed by UPLC assay. Streptococcus mutans, and Porphyromonas gingivalis were used to confirm the antibacterial effect of the ginger compounds and MC3T3-E1 cells were used to identify biocompatibility test. Cell viability and bacterial growth was determined by water-soluble tetrazolium salt (WST-8) colorimetric assay. Cellular morphology was identified with optical microscope after crystal violet staining. Cell differentiation and oxidative stress were evaluated by Alkaline phosphatase (ALP) assay and hydrogen peroxide colorimetric assay. The chemical bonding related with hydroxyl groups, carbonyl groups and aromatic ring was identified in all ginger compounds. Gingerol and shogaol presented good stability at acid and neutral pH at room temperature. All compounds showed better antibacterial effect against Porphyromonas gingivalis than Streptococcus mutans. 10-gingerol and all shogaol groups below 10-6 M presented suitable cytocompatibility for osteoblastic cells compared to control group. All groups showed similar Oxidative stress to control group, and ALP activity in all groups below 10-6 M was not statistically significant compared to control. Hence, this study concludes that shogaol groups presented better antibacterial effect and suitable cytocompatibility than gingerol groups.
초록
생강은 전 세계적으로 매운 음식과 전통 의학에서 사용되어지고 있다. 생강 내 페놀 화합물인 진저롤과 쇼가올은 세포 활성과 항균 효과를 가지고 있다고 알려져 있다. 본 연구의 목적은 6-, 8-, 10-gingerol과 6-, 8-, 10-shogaol이 조골세포에 대한 세포적합성과 대표적인 구강미생물들에 대한 항균효과를 조사하는 것이다. 진저롤과 쇼가올의 화학 구조는 FT-IR으로 분석하였으며, 온도와 pH에 따른 안정성은 UPLC로 분석하였다. Streptococcus mutans와 Porphyromonas gingivalis에 대한 생강 화합물의 항균특성을 확인하였고, MC3T3-E1 세포 적합성을 평가하였다. 세포 생존율 및 박테리아 성장은 WST-8 분석을 통해 평가하였다. 세포 형태학적 분석은 크리스탈 바이올렛 염색 후 광학현미경으로 관찰하였다. 조골세포의 분화와 산화 스트레스는 Alkaline phosphatase (ALP)와 H2O2 assay를 이용하여 평가하였다. 모든 생강 화합물 군에서 수산기, 카르보닐기 및 방향족 고리와 관련된 화학적 결합이 확인되었다. 진저롤과 쇼가올 군 모두 상온의 산성 및 중성 pH에서 우수한 안정성을 보였다. 또한 모든 생강 화합물은 Streptococcus mutans에 비해 Porphyromonas gingivalis에서 보다 우수한 항균효과를 보였다. 10-6 M 미만의 10-진지롤 및 모든 쇼가올 군들은 조골세포에 대해 세포독성을 보이지 않았다. 산화 스트레스는 모든 군에서 통계적으로 유의한 차이를 보이지 않았으며, ALP 활성은 10-6 M 농도 이하의 모든 군에서 정상 세포군과 유의한 차이를 보이지 않았다. 종합해보면 진저롤보다 쇼가올에서 더욱 우수한 항균특성 및 세포적합성이 확인되었다.
Keywords:
Ginger extract, Gingerol, Shogaol, Antibacterial activity, Cytocompatibility키워드:
생강 추출물, 진저롤, 쇼가올, 항균특성, 세포적합성Introduction
Ginger (Zingiber Officinale) is a member of the Zingiberaceae family and is frequently added to human consumption as a condiment, ginger rhizome has strong aroma and flavor, also pungent taste (1). It is also use as a remedy in traditional medicine system (2), and had been attributed therapeutic effect in treatment of diseases such as nausea, vomiting, asthma, palpitation, inflammation, rheumatism, hypertension, loss of appetite, digestion and pain (3, 4). More than 400 bioactive components have been detected in ginger rhizome including phenolic compounds, terpenes, polysaccharides, lipids, organic acids and oleoresins. However, the amount of the components found in ginger rhizomes vary depending on location, harvesting period, extraction method or drying method (5, 6). During in-vitro analyses of ginger extract effects have been found antimicrobial activity which can help in treatment of infections (7), bioactive molecules of ginger have shown scavenging activity against reactive oxygen species which can possibly prevent degenerative and aging process (8), including anti-inflammatory effect.
Fresh ginger flavor is due to volatile compounds of the essential oil and non-volatile oleoresin fraction. Among all the components found in ginger, the most bioactive compounds identified are phenolics and make up more than 10% composition on ginger rhizomes, mainly gingerols, zingerone and shogaols, these are also responsible for the pungent taste (9-11). Usually, the components found in greater quantity are 6-gingerol, followed by 8- and 10-gingerol (12), these are not stable as they generate the dehydration products shogaols which are more pungent constituents in dry ginger and the ratios of 6-, 8- and 10-shogaol found are variable depending on the dehydration process or storage (13).
Several studies have identified the bioactive components in ginger are effective decreasing the symptoms from chronic inflammatory diseases and possess antiinflammatory and antioxidant activity, as well as chemopreventive effects (14, 15). However, must of these studies focus on the exploration of 6-gingerol alone. On the other hand, some authors have identified the mechanisms of action of shogaols superior to gingerols. Swarnalaha et al (16), identified 6-shogaol as a promising compound with antioxidant and anti-inflammatory properties. Similarly, Ghasemzadeh et al (17), found higher radical scavenging ability on ginger extract with high shogaol content.
Ginger extract also has presented antimicrobial activity against pathogenic microorganisms such as Escherichia coli, Staphylococcus aureus and Candida albicans (18, 19). Isolated phenolic compounds, 10-gingerol and 12-gingerol evidenced potent antibacterial activity against anaerobic bacteria associated with human periodontitis (20). In contrast, antibacterial effect can be affected by application of different drying methods as Ghasemzadeh et al showed (17) the inhibitory effect of ginger extract can be related to higher shogaol content and different drying methods. For these reasons, ginger compounds are important substances for the study of their beneficial effects and can be sources of new therapeutically agents.
Oral floral is complex and diverse gram-negative and gram-positive microorganism interact in the development of diseases. The most common disease found in oral cavity is dental caries, which is mainly attributed to Streptococcus mutans as a primary etiologic agent (21, 22). Another important gram-negative anaerobe oral bacteria Porphyromonas gingivalis, which is considered one of the etiological factors in progressive periodontitis (23), another oral disease with high prevalence.
Therefore, the purpose of this study was to investigate the in-vitro cytotoxic effect on osteoblast cells (MC3T3-E1) and antibacterial effect of ginger phenolic compounds on the oral microorganisms, in an attempt to contribute to the use of these alternative products for oral microbial control and future development of dental materials. Qualitative spectra analysis of the main phenolic compounds was also carried out.
Materials and Methods
1. Materials
6-Gingerol, 8-Gingerol, 10-Gingerol, 6-Shogaol, 8-Shogaol and 10-Shogaol (≥ 98 purity, analysis of standard) were purchased from Chengdu Biopurity Phytochemicals Ltd (Sichuan, China). The other chemicals and reagents including ethanol, were of analytical grade and were purchased from Supleco Merck (Sigma-Aldrich Inc, Seoul, Korea).
2. Chemical structure analysis
For FT-IR analysis, the samples were prepared with the diluted concentrations at 10-2 M of 6-, 8-, 10-gingerol and 6-, 8-, 10-shogaol, one drop (10 μL) of solution was coated in platinum foil and let dry for 15 min, then the same process was repeated two more time and finally let dry overnight. The coated platinum foil was transported in 24 well plate.
The chemical structures of 6-, 8-, 10-gingerol and 6-, 8-, 10-shogaol were determined with a Fourier transform infrared (FT-IR) spectrophotometer (Perkin Elmer Frontier, Waltham, MA, USA) in the range from 4000 to 400 cm-1.
3. Thermal and pH stability assay
6-, 8-, 10-gingerol and 6-, 8-, 10-shogaol were prepared in analytical grade methanol (Merck, Darmstadt, Germany). An optimized selected ion recording (SIR) method was developed using Ulta-Performance Liquid chromatography (UPLC) coupled with tandem mass spectrometry (MS/MS). An UPLC system (Acquity system, Watrers, Milford, USA) was coupled to a Xevo TQ-S triple quadrupole mass spectrometer (Watrers, Milford, USA). Chromatographic separations were carried out using revers phase hybrid column (Synergi Hydro-RP, 4 μm; Phenomenex, CA, USA) maintained at 30 ℃. MS analysis was performed using the selected ion recording (SIR) mode by monitoring the of m/z 277.04. for 6-gingerol and 6-shogaol, m/z 305.14 for 8-gingerol and 8-shogaol, and m/z 332.99 for 10-gingerol and 10-shogaol. The gas flow of dissolution, cone and nebulizer were set at 650 L/Hr, 150 L/Hr and 7 bar, respectively.
4. Preparation of bacterial strains
Streptococcus mutans KCT3065 (S. mutans) and Porphyromonas gingivalis KCTC5352 (P. gingivalis) were used for antibacterial activity test in this study, which were acquired from Korean Collection for Type Cultures (KCTC, Jeollabuk-do, Korea).
First, the strains were incubated in a sheep blood agar plate (BAP, BANDIO Bio Science, Gyeonggi-do, Korea) at 37 ℃ in 5% CO2 atmospheres for 1 day, except for P. gingivalis which was incubated under anaerobic conditions for 7 days. Brain Heart Infusion (BHI, Becton, Dickinson and Co, Seoul, Korea) was inoculated with one colony of fresh pre-cultured dish and optical density was measure using DensiChek plus (Biomérieux, SA) until lecture reached 0.5, then 1 mL of this bacteria suspension was diluted in BHI (1:10 ratio) and this inoculum was used for the test (1.5×107 CFU/mL).
5. Antibacterial activity test
The minimum inhibitory concentration (MIC) of gingerols and shogaols was determined by microbroth dilution method using 96-well plates. 6-, 8-, 10-gingerol and 6-, 8- 10-shogaol subsequently serial dilution was performed to obtain the concentrations of 2×10-9 to 2× 10-2 M. Aliquots of 100 μL inoculums of each bacteria were added to all wells plate and finally incubated at 37 ℃ in 5% CO2 atmospheres for 1 day, except for P. gingivalis which was incubated under anaerobic conditions for 7 days. Three wells containing only medium were included for control group in each test. The absorbance after incubation was measured at a wavelength of 600 nm by a microplate reader (Emax Precision microplate reader, Molecular devices, USA). The lowest concentration which inhibited the growth of the bacteria was considered as the MIC.
6. Preparation of osteoblastic cells
Mouse osteoblastic MC3T3-E1 cells were purchased from American Type Culture Collection (Manassas, VA, USA), and were initially cultured in culture dish at 37 ℃ in 5% CO2 atmosphere in α-modified minimum essential medium (α-MEM; Thermo Fisher Scientific, Grand Island, USA). Unless otherwise specified, the medium contained 10% fetal bovine serum (FBS, Gibco Co., USA), 100 U/mL penicillin (Gibco Co., USA) and 100 μg/mL streptomycin (Gibco Co., USA). When cells reached 80% confluency, cells were seeded at a density of 2×104 cells/mL in 48-well plate with culture medium containing 6-, 8-, 10-gingerol and 6-, 8-, 10-shogaol representing six groups, every group was diluted in seven concentrations (10-3, 10-4, 10-5, 10-6, 10-7, 10-8 and 10-9 M) and incubated at 37 ℃ in a humidified 5% CO2 atmosphere for 1, 3 and 7 days.
7. Cell viability assay
Cell viability was determined 1 and 3 days after treatment. This method is based on the reduction of the tetrazolium salt WST-8 (2-(2-methoxy-4-nitrophenyl)-5-(2,4-disulfophenyl)-2H-tetrazolium, monosodium salt) by dehydrogenase activities in cells to give an orange-color formazan dye. Briefly, the viability assay was performed following the procedure described by the manufacturer using Cell Counting Kit-8 (CCK-8, Enzo, Farmingdale, NY), the medium was removed and washed with phosphatase buffer saline (PBS), then 500 μL WST-8 dye was added to each well, and incubated for 1 h at 37 ℃, finally media was transferred to 96 well plate (200 μL) and the absorbance was read at 450 nm in a microplate reader (Emax Precision microplate reader, Molecular Devices, CA, USA).
8. Cell-morphological analysis
Crystal violet staining was used to determine the effect of 6-, 8-, 10-gingerol and 6-, 8-, 10-shogaol on cells proliferation and morphology treated at different concentrations. MC3T3-E1 cells were cultured in 48-well plate for 1 and 3 days at 37 ℃ in 5% CO2 atmosphere before crystal violet assay was performed. This stain binds to DNA and proteins in cells on attached cells. Briefly, the medium was removed and cells were washed with PBS, this washed off non-adherent death cells, then adherent cells were fixed for 20 min with fixation solution (500 μL), containing 3% formaldehyde and 0.2% glutaraldehyde in PBS. Fixation solution was removed and washed with PBS and cells were stained with 0.5% (w/v) crystal violet solution (500 μL) for 20 min. Finally, cells were washed with PBS and air-dry at room temperature (RT) overnight. Stained cells were observed under optical microscope (DM2500M, Leica, Germany).
9. Alkaline phosphatase (ALP) activity assay
ALP activity was measured after 7 days of incubation by analyzing the rate of p-nitrophenyl phosphate (pNPP) hydrolysis using ALP assay kit (Takara Biotechnology, Shiba, Japan) according to protocol described by the manufacturer. Briefly, the medium was removed and wells were washed with saline solution, then were incubated in 100 μL ALP buffer (0.2 M Tris-HCI, Takara) and 100 μL pNPP solution (Takara) at 37 ℃ for 60 min in the dark. Then 100 μL 0.5 N Sodium hydroxide (NaOH, Showa, Korea) was added to each well to stop the reaction, finally the solution was transferred to 96-well plate and absorbance of the reaction was measured at 405 nm in a microplate reader (Emax Precision microplate reader, Molecular Devices, CA, USA).
10. Oxidative stress assay
After 7 days, the effect of 6-, 8-, 10-gingerol and 6-, 8-, 10-shogaol on cells oxidative stress by hydrogen peroxide (H2O2) production was determined by H2O2 colorimetric assay kit (BioVision Incorporated, Milpitas, USA) according to protocol described by the manufacturer. Briefly, the medium was transferred to 96-well plate and assay reagent (50 μL) was added, then incubated for 10 min at RT and absorbance was measured at 570 nm using a microplate reader. The H2O2 concentration was calibrated by a concurrently produced standard curve with standard solution (H2O2 standard 0.1 mM) at 0 μL, 10 μL, 20 μL, 30 μL, 40 μL and 50 μL, prepared according to instruction provided on the assay kit.
11. Statistical analysis
Quantitative data were expressed as the mean ± standard deviation (SD). One-way ANOVA and Tukey’s post hoc test were used to determine the level of significance in comparison to control group. A value of p<0.05 was considered to be significant.
Results
1. Chemical composition
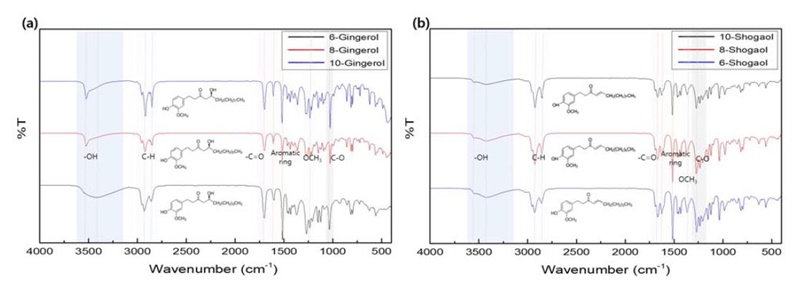
Figure 1 shows FT-IR spectra of gingerol and shogaol. The prominent absorption bands at approximately 3500 cm-1 for gingerol and shogaol indicated the hydroxyl group (-OH), and the peaks near 1700 cm-1 for gingerol and near 1666 cm-1 for shogaol indicated the presence of carbonyl group (-C=O). Meanwhile, the aromatic ring peak is observed at 1608 cm-1 for gingerol, at 1625 cm-1 for shogaol, and strong peak at 1515 cm-1 for both. Stretching peaks of C-H between 2800 and 3000 cm-1 in both. Finally, the peaks at approximately 1231 cm-1 were assigned to OCH3 for gingerol, C-O group was assigned near the peak 1270 cm-1 for shogaol and near peak 1025 cm-1 for gingerol.
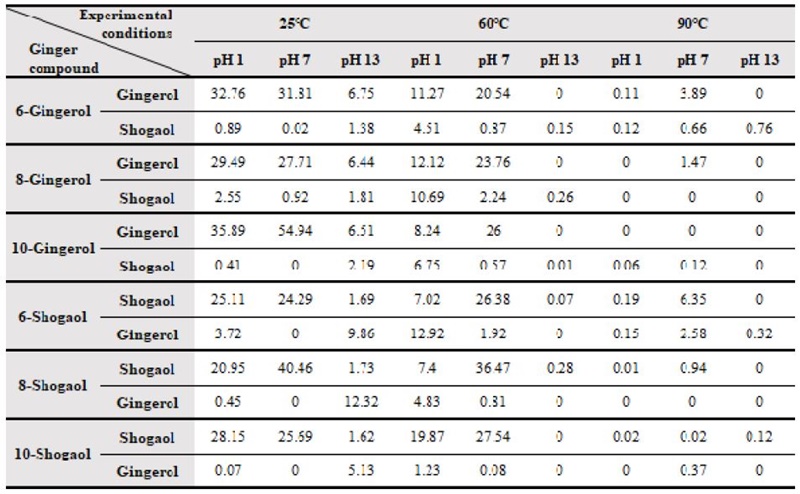
2. pH and thermal stability of gingerol and shogaol
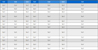
The effect on gingerol and shogaol stability of content in the sample was measure at different temperatures and pH (Table 1). Gingerol and shogaol presented the good stability at acid and neutral pH at the room temperature, however both compounds were unstable at alkaline pH and high temperature over 60 ℃. The increase in temperature affected the stability of content in the solutions, being more remarkable at 90 ℃ at this the solutions presented the lowest or inexistent content of ginger compounds with the exception of 6-shogaol and 6-gingerol that showed 6.35 and 3.89 ppm, respectively at neutral pH. At 60 ℃ in acid pH the content of shogaols increased in gingerols groups specially in 8-gingerol, yet this was observed at alkaline pH in shogaol groups increased the content of gingerol at lowest temperature, with the exception of 6-shogaol, in this groups gingerol content increased at acid pH at 60 ℃.
3. Minimum Inhibitory Concentration (MIC)
Figure 2 showed that the compounds had the antibacterial activity against S. mutans and P. gingivalis. Shogaols presented better inhibitory effects than gingerols against S. mutans and P. gingivalis, this last one was more sensitive. Bacteria growth in S. mutans was significantly inhibited at 10-2 M with 8-, 10-gingerol and 8-shogaol; 10-shogaol showed significant inhibition at 10-3 M.
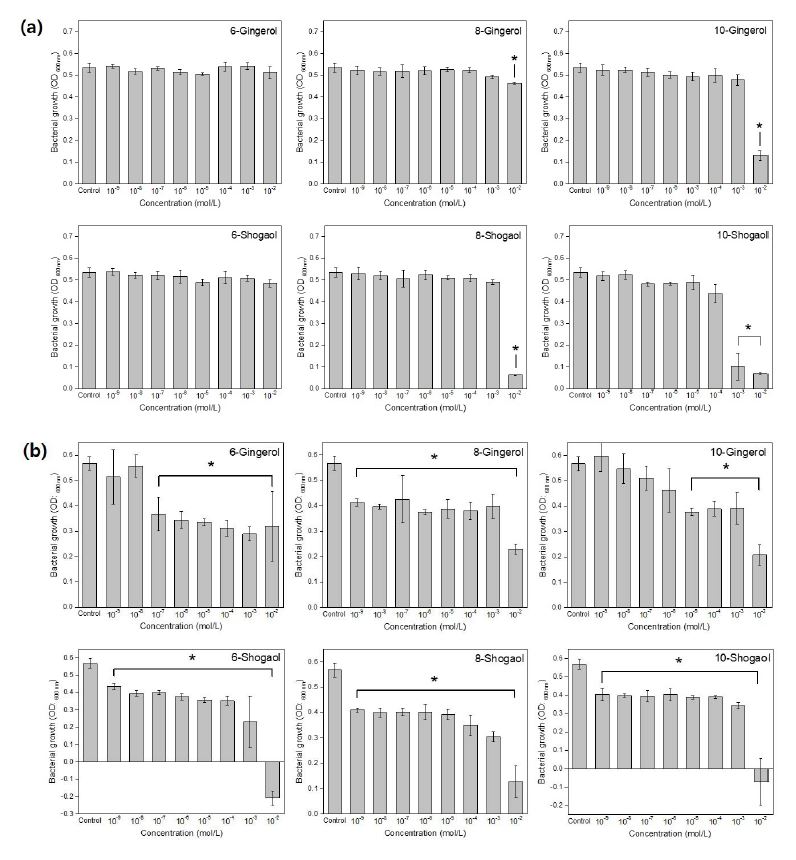
Bacterial growth of (a) S. mutans after 24 h treatment, and (b) P. gingivalis after 7 days of treatment with 6-, 8-, 10--gingerol and 6-, 8-, 10-shogaol at different concentrations in comparison to control group*There is significant difference in comparison to control group (p<0.05).
In the case of P. gingivalis the effectiveness was easily perceived in all compounds and concentrations, the most effective inhibition was observed with 8-gingerol, and all shogaols (p<0.05) at all concentrations. Meanwhile, 6-gingerol presented significant inhibitory effect above 10-7 M and 10-gingerol at concentrations above 10-5 M.
4. Effects of Gingerol and Shogaol on osteoblast viability and proliferation
The effect of shogaol and gingerol on osteoblast viability was assessed using WST-8 assay (Figure 3 (a)). After 1 day of treatment, 10-gingerol and all shogaol groups presented significant improvement (p<0.05) in osteoblast viability at lowest concentrations (below 10-7 M). After 3 days of treatment 6- and 8-gingerol presented higher toxicity (p<0.05) in all concentrations. Finally, it was observed that 10-gingerol, 6- and 10-shogaol groups presented better cell viability below 10-6 M concentrations.
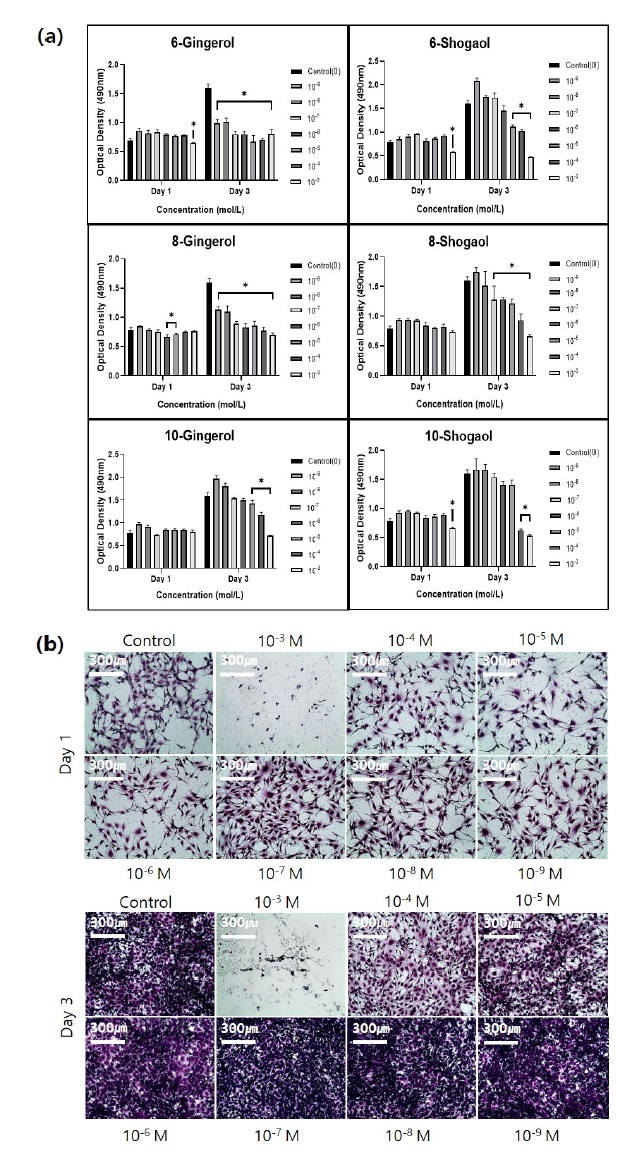
Osteoblast viability test with 6-, 8-, 10-gingerol, and 6-, 8-, 10-shogaol after (a) 1 day and 3 days of treatment at different concentrations. (b) Crystal violet dyed after 1 and 3 days of treatment with 6-shogaol.*There is significant difference in comparison to control group (p<0.05).
Osteoblast dyed with Crystal violet stain observed under microscope at day 3 (Figure 3 (b)), shown evident decrease on osteoblast proliferation effect above 10-5 M concentration in comparison to control group, as well osteoblast showed a marked shrinkage and an increased irregularity of the cell surfaces, while osteoblast proliferation effect was similar to control below 10-6 M concentration.
5. Oxidative stress assay
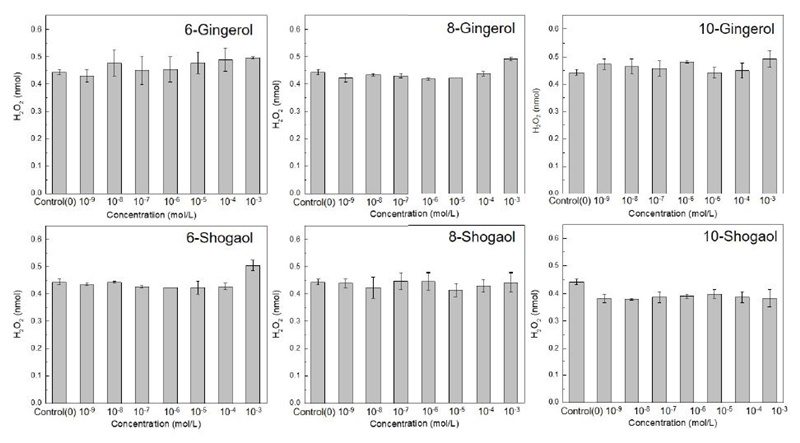
The direct effect of 6-, 8- and 10-gingerol and 6-, 8-and 10-shogaol on osteoblast oxidative stress by hydrogen peroxide (H2O2) production, was performed by H2O2 colorimetric assay. As shown in Figure 4, there was no statistically significant difference on H2O2 production between all groups and concentrations in comparison to untreated group (control).
6. Osteoblast differentiation assay
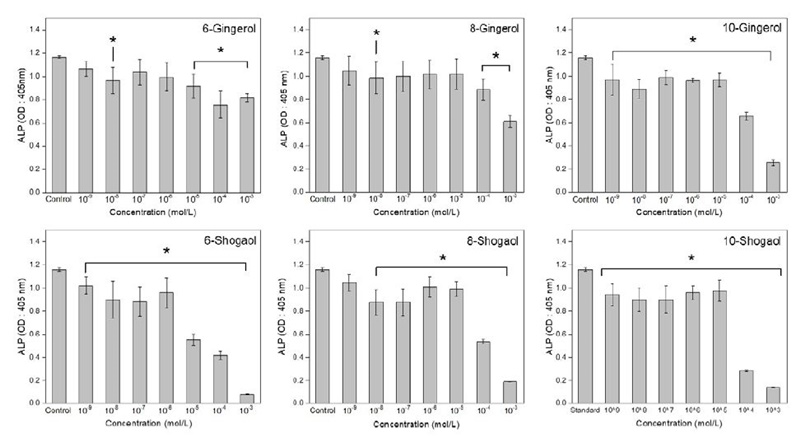
The measurement of Alkaline Phosphatase production by MC3T3-E1 cells cultured in the presence of shogaols and gingerols in different concentrations was performed using ALP assay. In Figure 5, it was found no difference in calcification activity in osteoblast after treatment with 6- and 8-gingerol at concentrations below 10-6 M. Alkaline phosphatase activity decreased in comparison to control group after treatment with 10-gingerol, and shogaol groups at all concentrations.
Discussion
In the present study, the FT-IR spectrum of gingerol and shogaol groups presented similar location to the main phytochemical compounds in ginger extract. However, some of the bands and peaks intensity changed in between each group and analog. The changes of intensity peaks in the present study could be related with the chemical difference native to every compound and the expression of each functional groups and bonding characteristics. One clear difference observed is related to –OH band intensity difference between gingerol groups and shogaol groups, which are the dehydrated form of gingerols after extraction drying method. Gingerol have been found instable at high temperatures, solar light and hot air (17, 24). This is observed at the -OH band intensity decreased in shogaol groups.
During the thermal stability test, the dehydration of gingerol groups at 60 ℃ resulted in production of shogaols which was higher than shogaols observed in gingerol groups at lower temperature. This was observed in the study of Gopi et al (25), in which at higher temperatures the gingerols converted to the corresponding shogaols. Also, the pH had influenced the dehydration of gingerol to form shogaol, and rehydration of shogaol to form gingerol which is better observed in 6-shogaol at 60 ℃ in acid pH. Bhattarai et al (26), observed the dehydration of gingerol and rehydration of shogaol at acid pH in higher temperatures, a reversible kinetic of the compounds in acid aqueous solution.
Plants and herbs antimicrobial activity is believed to be due their phytochemicals compounds, phenolic compounds and essential oils, this plants extracts had shown activity against microbial strains and possible substitution of drugs (27). Ginger rhizome crude extract antibacterial activity had been previous study and presented inhibitory effect against multi-drug resistant pathogens (7, 28). In this study the most effective antibacterial compounds were 6-, 8- and 10-shogaol at all concentrations specially against P. gingivalis, which was cultured for longer period of time, these compounds could inhibit the growth of the bacteria at lower concentrations also 6- and 10-shogaol exhibited antibacterial activity at the higher concentration (10-2 M). Bacterial growth inhibition against this pathogen was also observed by Park et al (20), resulting shogaol activity more effective than gingerol compounds against periodontal pathogens. S. mutans also presented sensitivity at higher concentrations of 8-, 10-gingerol and 8-, 10-shogaol after treatment for 24 hours. The essential oil of ginger had also showed inhibitory effect against S. mutans and ability to destroy it biofilm formation, it is also effective against other oral pathogens (29, 30). The phytochemical compounds of ginger extract shown antibacterial activity and possibilities to be used as therapeutic antimicrobial agents in oral infections.
To test cytotoxic cellular effect MC3T3-E1 cells were used, which are pre-osteoblastics cells that undergo osteoblastic differentiation. The results presented in figure 3 (a) shown no toxic effect of compounds after 1 day of treatment, and improvement in cellular viability at lowest concentrations (below 10-6 M) of 10-gingerol and all shogaol compounds after 3 days. In contrasts, Kim et al (31), studied the effect of 6-gingerol which presented no toxic effect at similar concentrations (10-9-10-7 M) after treatment for 2 days. The toxic effect can be reflected in the Crystal violet image presented in figure 3 (b) with the representative group treated with 6-shogaol, is observed low proliferation and cellular shrinkage at higher concentrations, 10-3 M at 1 day and above 10-5 M at 3 days. No study to compare these images have been found.
Ginger rhizome phytochemicals have also been attributed antioxidant scavenging capacity, Ammar et al (32), findings suggested this ability to the phenolic content in ginger extract overall 6-gingerol and 6-shogaol which showed better antioxidant ability than the extract alone. In contrast in this study the scavenging effect on osteoblastic cells analyzed by peroxide hydrogen production assay after treatment with gingerol and shogaol solutions presented no difference between groups and concentrations production in comparison to control group, these results could be affected by the long period of experiment test which could affect the effectiveness of the solutions. However, is remarkable to mention there is no correlation observed between peroxide hydrogen cellular production and toxicity on the samples viability test which could imply cellular apoptosis is not associated to cellular oxidation in this study.
On the other hand, other authors have studied the relationship between oxidative stress and inhibition of osteoblastic cells differentiation (33, 34). For this reason, oxidative stress and osteoblast differentiation were tested under similar conditions and period of time. Alkaline Phosphatase, is a bone-type alkaline necessary in the formation and calcification of hard tissue found in osteoblastic cells (35). To investigate gingerol and shogaol compounds effect on osteoblast function ALP activity was determined after 7 days, 6- and 8-gingerol did no showed significant difference of ALP production at lowest concentrations in comparison to control group, however, the other tested compounds presented significant decreased of ALP activity in all concentration even though cell viability was similar or better with these solutions. These results contrast with the study of Kim et al (31), the only compound under study was 6-gingerol which presented significant decreased cellular ALP activity. Although the exact mechanism that affect ALP activity in osteoblastic cells was not tested in this study, this was one limitation and requires future investigation.
In summary, this in-vitro results suggest that gingerol and shogaol presented in-vitro antibacterial activity and suitable cytocompatibility on osteoblastic cells, which may be promising for future investigations to use them as alternative products for oral microbial control and development of dental materials. However, further studies are needed to step forward.
Conclusion
In this study FT-IR spectrum expressed same functional groups in shogaol and gingerol tested solutions with differences in wavelength intensity, particularly observed in the –OH group band in shogaol groups. The theory of dehydration process in gingerols was also observed in the thermal stability test, in which temperature and pH affected each compound and caused dehydration in gingerol groups increasing shogaol content. It was found that 10-gingerol and all shogaols presented antibacterial activity in-vitro against oral bacteria (gram-negative) under study, with potent effect against P. gingivalis. Also, these ginger phytochemicals possess suitable cytocompatibility similar to control group for osteoblastic cell in concentrations below 10-6 M. However, ALP activity decreased in osteoblast cells after treatment for 7 days with these solutions at all concentrations. For these reasons, further studies are needed to elucidate the mechanism by which gingerols and shogaols affect osteoblastic differentiation. These results could provide valuable information for the relevant concentration range of gingerols and shogaols for development of biocompatible dental materials.
Acknowledgments
This work was carried out with the support of “Cooperative Research Program for Agriculture Science and Technology Development (Project No. PJ01520002)” Rural Development Administration, Republic of Korea.
References
-
Surth YJ. Molecular mechanisms of chemopreventive effects of selected dietary and medicinal phenolic substances. Mutat Res. 1999;428(1999):305-27.
[https://doi.org/10.1016/S1383-5742(99)00057-5]

-
Dong J. The Relationship between Traditional Chinese Medicine and Modern Medicine. Evid Based Complement Alternat Med. 2013;Article ID 153148:10 pages.
[https://doi.org/10.1155/2013/153148]

-
Baliga MS, Haniadka R, Pereira MM, D'Souza JJ, Pallaty PL, Bhat HP, et al. Update on the chemopreventive effects of ginger and its phytochemicals. Crit Rev Food Sci Nutr. 2011;51(6):499-523.
[https://doi.org/10.1080/10408391003698669]

-
Funk JL, Frye JB, Oyarzo JN, Timmermann BN. Comparative effects of two Gingerol-containing Zingiber Officinale extracts on experimental Rheumatoid Arthritis. J Nat Prod. 2009;72(3):403-07.
[https://doi.org/10.1021/np8006183]

-
Ghasemzadeh A, Jaafar HZ, Rahmat A. Variation of the Phytochemical Constituents and Antioxidant Activities of Zingiber officinale var. rubrum Theilade Associated with Different Drying Methods and Polyphenol Oxidase Activity. Molecules. 2016;21(6):780.
[https://doi.org/10.3390/molecules21060780]

-
Yeh HY, Chuang CH, Chen HC, Wan CJ, Chen TL, Lin LY. Bioactive components analysis of two various gingers (Zingiber officinale Roscoe) and antioxidant effect of ginger extracts. LWT - Food Sci Technol. 2014;55(1):329-34.
[https://doi.org/10.1016/j.lwt.2013.08.003]

-
Mohammed WF, Saleh BH, Ibrahim RN, Hassan MB. Antibacterial activity of Zingiber officinale (Ginger) against clinical bacterial isolates. SAJRM. 2019;3(2):1-7.
[https://doi.org/10.9734/sajrm/2019/v3i230080]

-
Kabuto H, Nishizawa M, Tada M, Higashio C, Shishibori T, Kohno M. Zingerone [4-(4-hydroxy-3-methoxyphenyl)-2-butanone] prevents 6-hydroxydo-pamine-induced dopamine depression in mouse striatum and increases superoxide scavenging activity in serum. Neurochem Res. 2005;30(3):325-32.
[https://doi.org/10.1007/s11064-005-2606-3]

-
Ma RH, Ni ZJ, Zhu YY, Thakur K, Zhang F, Zhang YY, et al. A recent update on the multifaceted health benefits associated with ginger and its bioactive components. Food Funct. 2021;12(2):519-42.
[https://doi.org/10.1039/D0FO02834G]

-
He XG, Bernart MW, Lian LZ, Lin LZ. High-performance liquid chromatography-electospray mass spectrometic analysis of pungent onsttuents of ginger. J Chromatogr A. 1998;796(2):327-34.
[https://doi.org/10.1016/S0021-9673(97)01013-3]

-
Ghasemzadeh A, Jaafar HZ, Rahmat A. Antioxidant activities, total phenolics and flavonoids content in two varieties of Malaysia young ginger (Zingiber officinale Roscoe). Molecules. 2010;15(6):4324-33.
[https://doi.org/10.3390/molecules15064324]

-
Lei L, Liu Y, Wang X, Jiao R, Ma KY, Li YM, et al. Plasma cholesterol-lowering activity of gingerol- and shogaol-enriched extract is mediated by increasing sterol excretion. J Agric Food Chem. 2014;62(43):10515-21.
[https://doi.org/10.1021/jf5043344]

- Ko MJ, Nam HH, Chung MS. Optimization of drying conditions for the conversion of 6-gingerol to 6-shogaol under subcritical water extraction from ginger. Korean J Food Sci Technol. 2019;51(5):447-51.
-
Kim EC, Min JK, Kim TY, Lee SJ, Yang HO, Han S, et al. [6]-Gingerol, a pungent ingredient of ginger, inhibits angiogenesis in vitro and in vivo. Biochem Biophys Res Commun. 2005;335(2):300-8.
[https://doi.org/10.1016/j.bbrc.2005.07.076]

-
Choi YY, Kim MH, Hong J, Kim SH, Yang WM. Dried Ginger (Zingiber officinalis) Inhibits Inflammation in a Lipopolysaccharide-Induced Mouse Model. Evid Based Complement Alternat Med. 2013;Article ID 914563:9 pages.
[https://doi.org/10.1155/2013/914563]

-
Dugasani S, Pichika MR, Nadarajah VD, Balijepalli MK, Tandra S, Korlakunta JN. Comparative antioxidant and anti-inflammatory effects of [6]-gingerol, [8]-gingerol, [10]-gingerol and [6]-shogaol. J Ethnopharmacol. 2010;127(2):515-20.
[https://doi.org/10.1016/j.jep.2009.10.004]

-
Ghasemzadeh A, Jaafar HZE, Baghdadi A, Tayebi-Meigooni A. Formation of 6-, 8- and 10-Shogaol in Ginger through application of different drying methods: Altered antioxidant and antimicrobial activity. Molecules. 2018;23(7):1646.
[https://doi.org/10.3390/molecules23071646]

- Yassen D, Ibrahim AE. Antibacterial activity of crude extracts of ginger (Zingiber officinae Roscoe) on Eschericia coli and Staphylococcus aureus: A study in vitro. IAJPR. 2016;6(06):5830-5.
-
Lee JH, Kim YG, Choi P, Ham J, Park JG, Lee J. Antibiofilm and Antivirulence Activities of 6-Gingerol and 6-Shogaol Against Candida albicans Due to Hyphal Inhibition. Front Cell Infect Microbiol. 2018;8:299.
[https://doi.org/10.3389/fcimb.2018.00299]

-
Park M, Bae J, Lee DS. Antibacterial activity of [10]-gingerol and [12]-gingerol isolated from ginger rhizome against periodontal bacteria. Phytother Res. 2008;22(11):1446-9.
[https://doi.org/10.1002/ptr.2473]

-
Loesche WJ. Role of Streptococcus mutans in Human Dental Decay. Microbiol Rev. 1986;50(4):353-80.
[https://doi.org/10.1128/mr.50.4.353-380.1986]

-
Ahmad KA, GBD 2017. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. The Lancet. 2018;392(10159):1789-858.
[https://doi.org/10.1016/S0140-6736(18)32279-7]

-
Bostanci N, Belibasakis GN. Porphyromonas gingivalis: an invasive and evasive opportunistic oral pathogen. FEMS Microbiol Lett. 2012;333(1):1-9.
[https://doi.org/10.1111/j.1574-6968.2012.02579.x]

-
Ko MJ, Nam HH, Chung MS. Conversion of 6-gingerol to 6-shogaol in ginger (Zingiber officinale) pulp and peel during subcritical water extraction. Food Chem. 2019;270(1):149-55.
[https://doi.org/10.1016/j.foodchem.2018.07.078]

- Gopi S, Varma K, Jude S. Study on temperature dependent conversion of active components of ginger. Int J Pharma Sci. 2016;6(1):1344-1347.
-
Bhattarai S, Tran VH, Duke CC. The stability of Gingerol and Shogaol in aqueous solutions. J Pharm Sci. 2001;90(10):1658-64.
[https://doi.org/10.1002/jps.1116]

-
Teixeira B, Marques A, Ramos C, Neng NR, Nogueira JMF, Saraiva JA, et al. Chemical composition and antibacterial and antioxidant properties of commercial essential oils. Ind Crops Prod. 2013;43:587-95.
[https://doi.org/10.1016/j.indcrop.2012.07.069]

-
Karuppiah P, Rajaram S. Antibacterial effect of Allium sativum cloves and Zingiber officinale rhizomes against multiple-drug resistant clinical pathogens. Asian Pac J Trop Biomed. 2012;2(8):597-601.
[https://doi.org/10.1016/S2221-1691(12)60104-X]

-
Mostafa NM. Antibacterial Activity of Ginger (Zingiber officinale) Leaves Essential Oil Nanoemulsion against the Cariogenic Streptococcus mutans. J Applied Pharma Sci. 2018;8(9):34-41.
[https://doi.org/10.7324/JAPS.2018.8906]

- Pillay SR, Roy A, Rajeshkumar S, Lakshmi T. Antimicrobial activity of turmeric, cumin, and ginger oil on oral pathogens. Drug Invent Today. 2019;11(5):1106-1109.
- Young-Ho K, Tung NH, Yan D, Sang-Heock P, Eun-Mi C. Effect of [6]-gingerol, a pungent ingredient of ginger, on osteoblast response to extracellular reducing sugar. Food Sci Biotechnol. 2007;16(5):807-11.
-
Ali AMA, El-Nour MEM, Yagi SM. Total phenolic and flavonoid contents and antioxidant activity of ginger (Zingiber officinale Rosc.) rhizome, callus and callus treated with some elicitors. J Genet Eng Biotechnol. 2018;16(2):677-82.
[https://doi.org/10.1016/j.jgeb.2018.03.003]

-
Bai XC, Lu D, Bai J, Zheng H, Ke ZY, Li XM, Luo SQ. Oxidative stress inhibits osteoblastic differentiaiton of bone cells by ERK and NF-Kb. Biochem Biophys Res Commun. 2004:314(1):197-207.
[https://doi.org/10.1016/j.bbrc.2003.12.073]

-
Arai M, Shibata Y, Pugdee K, Abiko Y, Ogata Y. Effects of reactive oxygen species (ROS) on antioxidant system and osteoblastic differentiation in MC3T3-E1 cell. IUBMB life. 2007:59(1):27-33.
[https://doi.org/10.1080/15216540601156188]

-
Sugawara Y, Suzuki K, Koshikawa M, Ando M, Iida J. Necessity of Enzymatic activity of alkaline phosphatase for mineralization of osteoblastic cells. Jpn J Pharmacol. 2002;88(3):262-9.
[https://doi.org/10.1254/jjp.88.262]